Contents
Corneal ulcers, or ulcerated eyes and lids, occur when the eye becomes inflamed, resulting in an ulcer on the eyeball. The problem may then extend to the eyelid. Most likely, a corneal ulcer occurs because the usual covering of the eye was scratched or damaged and then became infected; the infection is generally caused by a virus. The ulcer can also be caused by blepharitis.
Causes of Corneal Ulcers
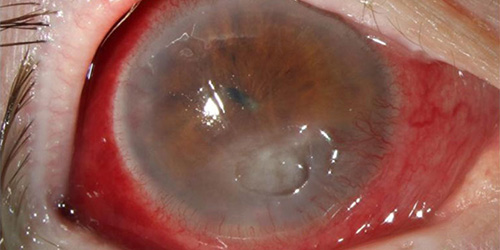
There are numerous factors, including the following, that can cause corneal ulcers:
- Bacterial, viral, or fungal diseases
- Staphylococcus aureus
- Pseudomonas aeruginosa
- herpes simplex virus
- Fungi like Candida
- Aspergillus
Trauma: Corneal ulcers can form when the cornea is injured, such as when something scratches your eye. This condition can also result from wearing dirty or damaged lenses, using contact lenses for an extended period, or misusing them.
Dry eye syndrome: The cornea can become dehydrated due to inadequate tear production or poor tear quality, increasing the risk of injury and ulceration.
Underlying medical conditions: Several systemic diseases, including autoimmune diseases and severe allergies, can raise the risk of corneal ulcers.
Symptoms of Ulcerated Eye and Lid
The following signs and symptoms could point to a corneal ulcer:
- Corneal ulcers frequently cause severe eye pain or discomfort, which may worsen when one blinks or is exposed to light.
- Redness and swelling: A continuing infection or inflammation may cause the affected eye to be red and swollen.
- Reduced or distorted vision: Corneal ulcers may cause visual abnormalities like vision or light sensitivity.
- The eyes can produce extra tears due to the discomfort and inflammation brought on by the corneal ulcer.
- Sandy or foreign body sensation in the eye: People who have corneal ulcers may have this sensation.
Treatment
An ulcerated eye and lid must be treated immediately to minimize complications and promote healing. Numerous treatments may be available based on the ulcer’s severity and underlying cause. Here are a few typical methods:
- Depending on the suspected cause of the corneal ulcer, your doctor may advise you to use eye drops that include antibiotics or antifungals to treat the underlying infection.
- Topical steroids: Corticosteroid eye drops may occasionally lessen inflammation and aid healing. However, their use should be carefully watched, as they can worsen some diseases.
- Bandage contact lens: A tailored soft contact lens can cover the cornea and aid healing by creating a barrier of protection and easing discomfort.
- Oral treatments: If the infection is severe or has progressed through the cornea, oral antibiotics or antifungal medications may be advised.
- Lubricating eye drops or ointments can relieve symptoms brought on by dry eyes and the dryness itself.
- Get plenty of rest, improve your diet, and take large doses of vitamin C (2000 mg, three times a day).
- Apply a warm yellow dock tea poultice to the eyelid. You can also drink it.
- Sometimes, your doctor may suggest surgery, particularly when the ulcer does not respond to conventional treatment or when complications arise. However, one procedure is corneal transplantation.
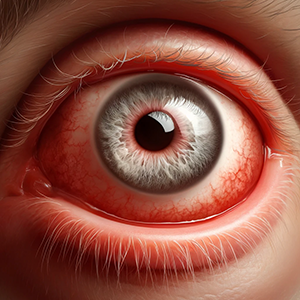
Prevention
Taking preventive measures is essential to reducing the risk of corneal ulcers. The following are some safety recommendations:
- Follow your eye doctor’s directions for cleaning, disinfecting, and wearing contact lenses for proper lens maintenance.
- Routine eye exams: Regular eye exams can help detect potential problems early and enable prompt management.
- Eye protection: When engaging in activities that may cause eye harm, wear the proper eye protection, such as safety goggles or glasses.
- Proper hand hygiene will help stop the spread of diseases that might cause corneal ulcers. The risk of infection increases when people share personal eye care items like towels, eye drops, or contact lenses.
- If not promptly treated, corneal ulcers can be uncomfortable and compromise eyesight. Successful management depends on knowing the reasons, identifying the symptoms, and getting help immediately.
- People can dramatically lower their chance of developing corneal ulcers and keep their vision in good condition by keeping their eyes clean, adopting safety precautions, and taking care of any eye-related issues as soon as they arise.
Health Disclaimer: The information on this website is for educational uses only and is not a substitute for professional medical advice. Always consult an authorized healthcare provider for any health concerns before using any herbal or natural remedy. We do not establish, treat, cure, or prevent any disease. Reliance on any material from this website is solely at your own risk. We are not responsible for any adverse effects resulting from the use of information or products mentioned on this website.
REFERENCES
- Vance Ferrell Harold M. Cherne, M.D. The Natural Remedies Encyclopedia [Book]. – Altamont, TN: Harvestime Books, 2010. – Vol. Seventh Edition: 7: pp. 395.
- American Academy of Ophthalmology: https://www.aao.org/eye-health/diseases/corneal-ulcer
- American Optometric Association: https://www.aoa.org/healthy-eyes/caring-for-your-eyes/diet-and-nutrition?sso=y
- World Health Organization: https://www.who.int/news-room/fact-sheets/detail/blindness-and-visual-impairment
- Nature Reviews Drug Discovery: https://www.nature.com/articles/nrd4482
