Shingles is a viral infection that creates painful rashes, appearing as a blister and developing on either side of the body. Although it can be found on any body part, it typically makes striped blisters on either side of the torso.

Shingles can happen to anyone, but they can be a more serious problem for seniors. It comes with a higher risk of stroke and more severe health complications, generally due to a weakened immune system that naturally occurs as we age. Seniors can find it more challenging to fight off any infection due to a weak immune system.
Shingles is not a life-threatening condition but can be very painful. The best way to avoid it is to get vaccinated against the virus. Although it is a treatable condition, it can still lead to further complications – postherpetic neuralgia being the most common.
Postherpetic neuralgia causes lingering pain even after the blisters have been treated or disappeared. Depending on which nerves in the body become affected, other complications from shingles can also develop, such as loss of vision, skin infections, and some neurological conditions.
Causes and Risk Factors
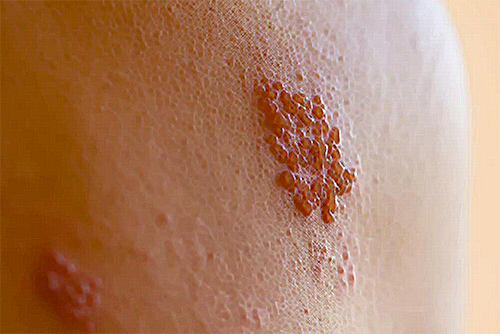
The leading cause of shingles is the varicella-zoster virus. This virus is also responsible for chickenpox. Once a person has been infected with chickenpox, the virus remains in the nerve tissues near the brain and the spinal cord, even once it becomes inactive. Several years later, it can reactivate again, travel the nerve pathways toward your skin, and then you feel the impact of shingles.
While there is a huge chance that one can develop shingles if they’ve had chickenpox in the past, not everyone infected with chickenpox develops shingles later on.
Other factors can also make a person more likely to develop shingles, including prolonged use of steroids, radiation, or chemotherapy, mostly over 50 years of age. The risk of developing shingles goes higher with age.
Symptoms and Signs
The most common symptom of shingles is pain. It may range from moderate to intense, but some people may only feel the pain and not develop a rash. If a rash develops, it usually appears as a stripe of blisters. They can appear on the body, around an eye, or on one side of the face or neck.
Shingles naturally affect a small area of the body at any given time. The most common signs and symptoms are:
- Painful and burning sensation.
- Itching.
- Sensitivity to touch, and if touched, it can be excruciating.
- Seeing red rashes appear even days after feeling pain.
- Fluid-filled blisters, similar to chickenpox.
- Sometimes, it can include other symptoms such as headache, fatigue, fever, and light sensitivity.
Treatment and Prevention
Shingles may be prevented with an antiviral vaccine. For older adults, a vaccine is recommended for prevention.
If shingles develop, medications are available to treat the infection. Successful treatment includes prompt response to the initial symptoms, proper medical evaluation, quick treatment of antiviral medications, and pain therapy if required. Prompt attention and action can go a long way in treating shingles effectively, especially if the person is elderly. Shingles may resolve on its own, even without treatment. However, the viral infection may need to be treated aggressively to prevent further complications.
Antiviral medication: Various types of antiviral medication for shingles are available, and your doctor will prescribe the one they think will best treat the shingles outbreak.
Pain medication: If the pain is mild, acetaminophen (Tylenol) or NSAIDs (ibuprofen or naproxen) may be safely given to seniors. However, opioid pain relievers or corticosteroids could be necessary if the pain is more intense. Doctors should medically prescribe pain medications to prevent further complications.
Alternate therapies: If the elderly prefer alternative pain management therapies, they can speak to their natural healthcare provider. They will provide treatment solutions or pain remedies suitable for their needs. Meditation training and regular mindfulness meditation could complement other pain management therapies.
Shingles should not be ignored, so see your doctor at the first sign of pain and discomfort. If you can prevent the virus from worsening, you will reduce both the intensity and the duration of the painful symptoms.
DISCLAIMER: All content on this website is presented solely for educational and informational objectives. Do not rely on the information provided as a replacement for advice, diagnosis, or treatment from a qualified medical expert. If you are pregnant, nursing, or have any preexisting medical concerns, talk to your doctor before using any herbal or natural medicines.
References
- Shingles (Herpes Zoster): https://www.cdc.gov/shingles
- What Everyone Should Know About Zoster Vaccine: https://www.cdc.gov/vaccines/vpd/shingles/public/shingrix/index.html
